Welcome to the Rivron Lab
The Rivron group recreates embryonic development using mammalian stem cells in a dish to better understand the encoded principles of self-organization.
Fish schools, ant colonies and bird flocks are complex systems that coordinate their collective behaviors to control the emergence and progression of patterns and functions. For example, fish in schools swim faster than individual animals are able to. This broad range of decentralized, adaptive behaviors based on local interactions is called self-organization. We explore how self-organization complements traditional hierarchical genetic (e.g., HOX genes collinearity) and molecular (e.g., morphogen gradients) processes to shape the mammalian organism.
The blastocyst is the early mammalian organism before implantation. It is a powerful model for self-organization because it is autonomous, adaptive, and small enough to be studied in great detail. Our lab created a unique model of the blastocyst, termed the blastoid, which is formed by the spontaneous organization of stem cells in a dish. Blastoids contain all three cell types that further develop into the complete organism (embryonic and extra-embryonic tissues), and implant when transferred in utero. Contrary to blastocysts, blastoids are versatile in that they facilitate the systematic modulation and analysis of the impact of cell numbers, states and communication mechanisms on development. Furthermore, blastoids are readily generated in large numbers, making them suitable for high-throughput genetic and drug screens.
We observe both blastocysts and blastoids to study how self-organization contributes to multicellular patterning and cellular decision making. We address these questions using high throughput microsystems, single cell genomics, single cell high-content imaging, and synthetic biology. Our lab is supported by a diverse array of world-class scientific facilities at the Vienna Biocenter ranging from stem cell genome engineering, single cell transcriptomic, mass spectrometry, high-throughput and high-content imaging, recombinant protein production, and others.
Vision
Our overall goal is to understand the principles that synchronize cells in space and time to shape the early mammalian embryo.
Mission
Opening the black box of early development.
We know very little about how early mammalian embryos form. This is partly due to their small size (the width of a hair) and the fact that they are inaccessible in the womb. Such knowledge is vital as minor flaws at the start of development can prevent embryos from implanting in utero and lead to infertility or generate a ripple of adverse effects that can cause sub-optimal pregnancies and contribute to chronic illness in adulthood (e.g., diabetes, cardiovascular disease). Our research improves the understanding of the path that an organism takes during early development.
Modeling with stem cells.
The blastocyst is a hollow sphere formed from about a hundred cells. It consists an outer layer of trophoblast cells (the future placenta), and a small inner cluster containing embryonic cells (the future embryo) and primitive endoderm cells (the future yolk sac). Stem cell lines representing these three lineages can be cultured independently, multiplied extensively, and genetically edited in the laboratory. Using high throughput microsystems, we have assembled stem cells under conditions favoring their conversation and spontaneous organisation into structures – which we term blastoids– morphologically and transcriptionally resembling E3.5 blastocysts. This approach allows us to more systematically modulate and analyse behaviours, and to run drug and genetic screens. Blastoids have proven to be a powerful stem cell-based model to investigate previously inaccessible principles of development.

A conversation between stem cells.
We observed that, like blastocysts, blastoids form as a result of multiple inductive signals that originate from the inner embryonic cells and drive the development of the outer trophectoderm. By genetically and physically uncoupling these populations, we showed that the embryonic cells maintain trophoblast stemness (proliferation and self-renewal), while driving trophoblast morphogenesis. Together, these embryonic inductions maintain the trophoblast cells in a state capable of implanting in utero. From these initial discoveries, we have so far concluded that the nascent embryo fuels the development and implantation of the trophectoderm.
In utero implantation.
Blastoids model the state before implantation in utero and contain analogs of the tissues (polar and mural trophectoderm) necessary to interact with the mother’s uterine wall. Therefore, we use blastoids to investigate the mechanisms that mediate the attachment and invasion into the uterine wall and the formation of the maternal cocoon. This phenomenon of implantation is absolutely crucial and often fails during human pregnancy (approximately 30% of human fertilized eggs naturally fail to implant (Norwitz et al. 2001)).
The blastocyst as a complex system.
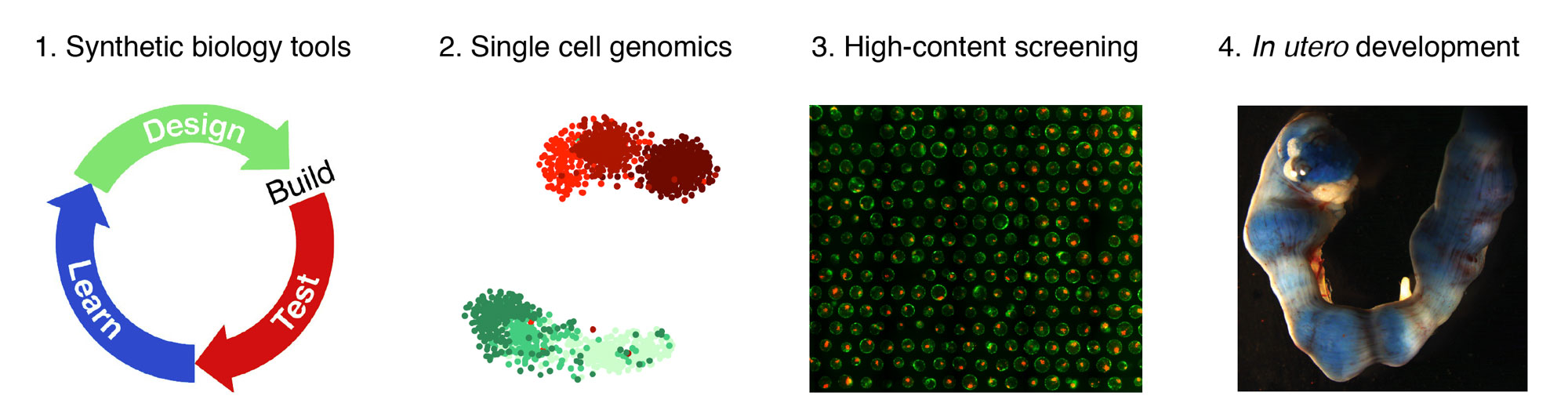
We use blastocysts and self-organizing models formed from stem cells, that we termed blastoids, to investigate how and why the flow of information between cells regulates spatio-temporal patterning and cell-fate decision making. This requires to consider blastocysts as complex systems from the viewpoint of physicists and engineers. We are a team of stem cell biologists, geneticists, synthetic biologists and engineers whose research is grounded in technological and computational approaches (e.g., microsystems, single cell sequencing, three-dimensional high content imaging) and collaborating with physicists.
Impact
The two sides of a coin: the management of infertility and contraception.
Around the world, pregnancy management is not optimal. Many women in developed countries are delaying the choice to have children until a later age, which has led to a decrease in fertility. In addition, new contraceptives that better adapt to populations and limit undesirable side-effects are required (see United Nation). Women must be able to better plan pregnancy without decreasing their chance of having a child. Family planning is essential to secure the autonomy and well-being of women, while also supporting the health and development of communities worldwide.
Understanding and managing the implantation into the uterus.
Successful management of pregnancy requires an understanding of the early events of development. This includes the formation of the trophectoderm, the tissue that mediates the implantation into the uterus, and its interaction with the uterine tissues (Cha, Sun, and Dey 2012), which defines both the beginning and often the success of pregnancy. In humans, at least 40% of natural pregnancies fail by 20 weeks, and 70% of those that fail do so at implantation (Norwitz et al. 2001). The steps of blastocyst development and implantation provide a window of opportunity to either enhance fertility or prevent pregnancy.
For example, only 20% of IVF procedures result in a birth, which is in part due to sub-optimal implantation (Chen et al. 2017). Understanding early development could help to optimize IVF culture medium (e.g., minimize chromosomal and cellular abnormalities). As well as safeguarding the health of children conceived in vitro (Chen et al. 2017), this could reduce the number of IVF procedures necessary for a successful pregnancy.
In vitro models from stem cells: an ethically and technically powerful choice.
Embryos are scarce, precious and should not be used lightly in research. This makes the study of infertility and contraception difficult. We use stem cells as an alternative to the use of blastocysts donated for research from in vitro fertilization (IVF) programs. Contrary to blastocysts, blastoids can be generated in large numbers and studied in greater detail. Our laboratory has shown that this model presents an exciting, albeit formidable, challenge to crack the code of early development, potentially contribute to the development of new medicines, and partially replace the use of animals and IVF blastocysts (Rivron NC, Pera M & al. 2018, Nature).
Ethics
Because blastoids are formed solely from stem cells, their use in research avoids ethical concerns surrounding the use of blastocysts. They represent an alternative scientific model to investigate early development and provide unique possibilities for high-throughput screens and fine modulations of cellular sub-populations, which are the basis of biomedical discovery. Blastoids are not considered to be a legal equivalent of blastocysts - they are laboratory models to study scientific and medical questions and represent an opportunity to investigate global health issues. The ethical aspects of our research are explained in Rivron, Pera et al. 2018.
Additional information at:
References
Burton, Graham J., Abigail L. Fowden, and Kent L. Thornburg. 2016. “Placental Origins of Chronic Disease.” Physiological Reviews 96 (4): 1509–65.
Cha, Jeeyeon, Xiaofei Sun, and Sudhansu K. Dey. 2012. “Mechanisms of Implantation: Strategies for Successful Pregnancy.” Nature Medicine 18 (12): 1754–67.
Chen, M., and L. K. Heilbronn. 2017. “The Health Outcomes of Human Offspring Conceived by Assisted Reproductive Technologies (ART).” Journal of Developmental Origins of Health and Disease.
Norwitz, E. R., D. J. Schust, and S. J. Fisher. 2001. “Implantation and the Survival of Early Pregnancy.” The New England Journal of Medicine 345 (19): 1400–1408.
Rivron, Nicolas. 2018. “Formation of Blastoids from Mouse Embryonic and Trophoblast Stem Cells,” May. DOI: doi.org/10.1038/protex.2018.051
Rivron, Nicolas C. [corresponding author], Javier Frias-Aldeguer, Erik J. Vrij, Jean-Charles Boisset, Jeroen Korving, Judith Vivié, Roman K. Truckenmüller, Alexander van Oudenaarden, Clemens A. van Blitterswijk [equal contribution], and Niels Geijsen [equal contribution]. 2018. “Blastocyst-like Structures Generated Solely from Stem Cells.” Nature 557 (7703): 106–11.
Selected Publications
Kagawa, H., Javali, A., Khoei, HH (...) David, L., Rivron, N. (2021). Human blastoids model blastocyst development and implantation. Nature.

HFSP Young Investigator
Human Frontier Science Program
