ReHIS Project
Refugee Health and Integration Survey:
Mental Health and Health Access of Refugees in Austria
Refugee Health and Integration Survey (ReHIS) is a study conducted by researchers from the Vienna University of Economics and Business (WU), the Vienna Institute of Demography of the Austrian Academy of Sciences (VID / ÖAW) and the Vienna Institute for International Economic Studies (wiiw) that provides data on refugees’ mental health and their access to health care Austria. Barriers to health access include accessibility, long waiting lists and a lack of information. Refugee women, people from Afghanistan and young refugees display low levels of physical and mental health. The authors recommend expanding mental health treatment programs in native languages.
Published in March 2019 in Health Policy, the study examines subjective well-being and access to public health care for refugees in Austria, one of the countries most heavily affected by the "refugee crisis" in 2015. It is based on primary data from ReHIS, a cross-sectional survey of 515 Syrian, Iraqi and Afghan refugee in Austria.
Four out of ten women report unmet health needs
The results show that refugees, especially women and people from Afghanistan, tend to rate their health poorer than the Austrian general population. Although respondents were very satisfied with the Austrian healthcare system, structural barriers to health access became evident, including lack of accessibility, insufficient number of places in treatment programs, lack of knowledge about doctors in the immediate environment and language barriers (Fig. 1).
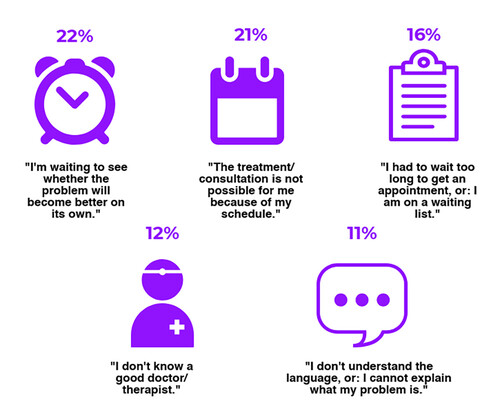
Two out of ten men and four out of ten women mentioned unmet health needs. Women also tend to assess their subjective well-being worse than men. This can be contributed, among other factors, to a generally high birth rate among recent refugees and resulting higher health care needs.
Forced migration affects health
On average, refugees from Afghanistan rate their health worse than refugees from Syria and Iraq. An essential factor for the heightened vulnerability of Afghans is their particular migration experience, which tends to be longer, more complex and fragmented than that of Syrians or Iraqis, with extended stays in transit countries. Furthermore, long asylum application processes, according inactivity and unemployment, and the fact that Afghans are typically only granted temporary subsidiary protection instead of full asylum status can contribute to their poorer state of health.
Hospitals more frequent than specialists
Although treatment costs were rarely cited as access barriers, respondents seldom used those health services that are typically associated with an additional financial contribution by the patient, such as preventive dental treatments (Fig. 2). This can be attributed to the fact that Information about available medical specialists is often difficult to access for refugees. Furthermore, hidden costs and language barriers may come into play. This is also reflected by the circumstance that respondents reported hospital treatment almost twice as often as Austrians, especially as outpatients (Fig. 2), where (web-based) interpreting services are more readily available.
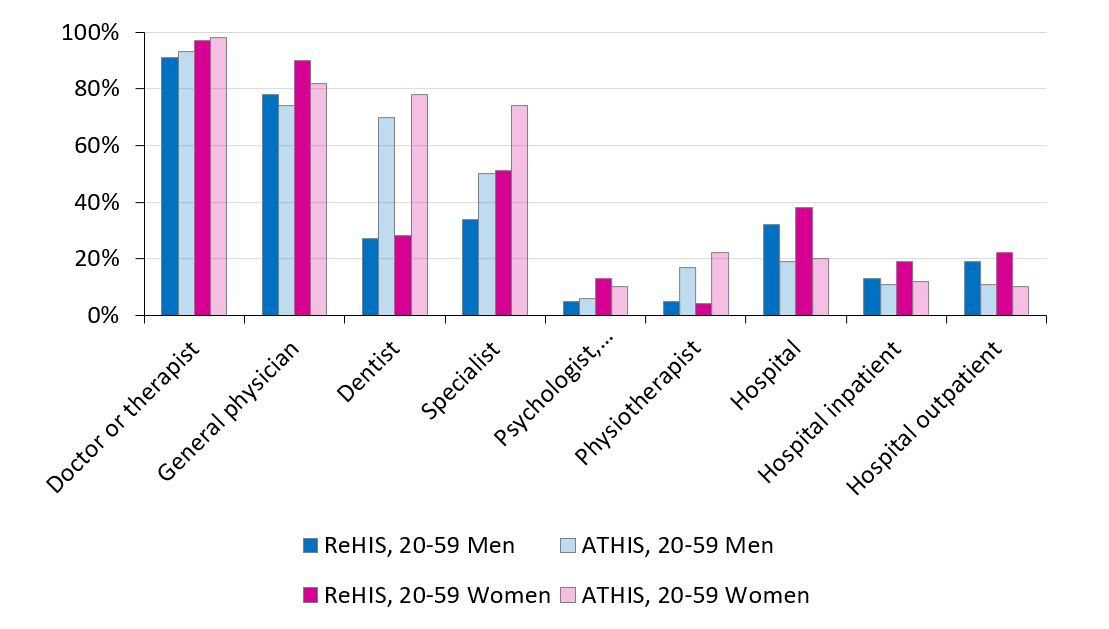
Need for mental health care
Results also suggest that the need for psychotherapy among refugees is much higher than among the Austrian general population. The prevalence of moderate and severe anxiety disorders and depression is about twice as high. In particular, adolescents and young adults aged 15-24 years reveal high levels of anxiety and depression symptoms (Fig. 3).
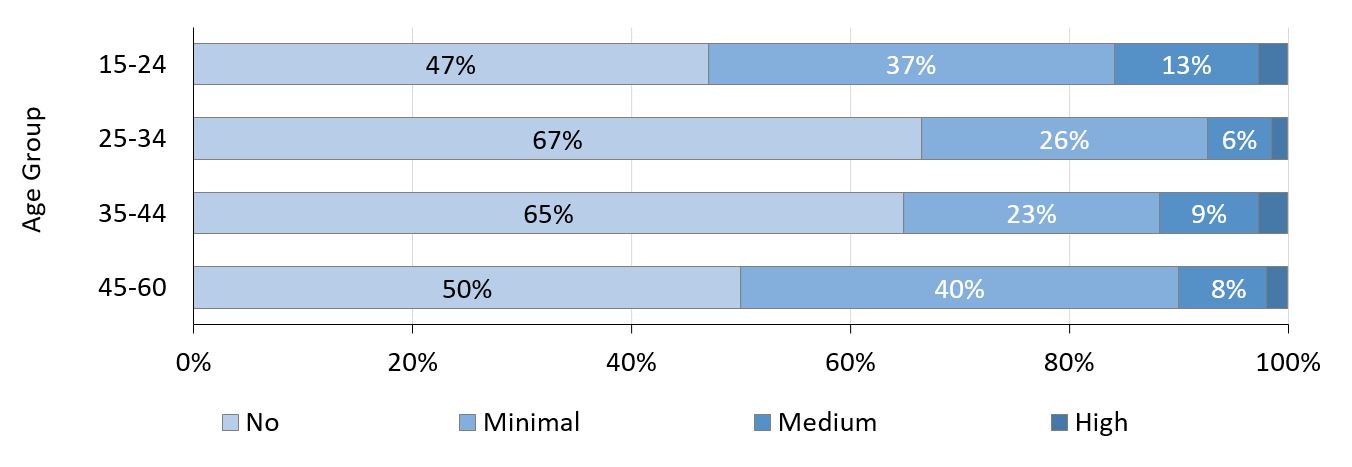
The study therefore recommends the expansion of mental health treatment programs in refugees’ native languages, in combination with mental health education, to counteract the widespread stigmatization of mental illness. Being affected by anxiety disorders and/or depression can be a major obstacle to learning new languages and integrating into society. The authors thus welcome the City of Vienna’s decision to increase funds for mental health programs such as Hemayat, which caters for the needs of traumatized refugees and torture victims.
About ReHIS
Between March and May 2018, more than 500 mainly Syrian, Iraqi and Afghan refugees were interviewed by telephone (CATI) in their first languages for the nationwide cross-sectional survey ReHIS. The questionnaire was based on established surveys such as EU SILC, the WHO Quality of Life Survey and the German IAB-BAMF-SOEP Refugee Survey. To assess the prevalence of depression and anxiety disorders, common clinical screening tools were used. Comparisons with the Austrian resident population are based on the Austrian Health Interview Survey (ATHIS 2014), which provides representative data on physical and mental health. ReHIS was funded by the Federal Ministry of Education, Science and Research, the Federal Ministry of Labour, Social Affairs, Health and Consumer Protection, the Fonds Soziales Wien, and the Common Health Goals of the “Rahmen-Pharmavertrag”, a cooperation between the Austrian pharmaceutical industry and the Austrian social insurance.


Publications
The effects of stressors and resiliance factors on mental health of recent refugees in Austria
Author(s): Leitner, S, Landesmann, M, Kohlenberger, J, Buber-Ennser, I and Rengs, B
Reference: wiiw Working Paper 169, Vienna: The Vienna Institute for International Economic Studies
Year: 2019
Was wissen wir über die Geflüchteten, die 2015 zu uns kamen?
Author(s): Buber-Ennser, I, Kohlenberger, J and Rengs, B.
Reference: J. Kohlbacher & M. Six-Hohenbalken (eds.) Die lange Dauer der Flucht – Analysen aus Wissenschaft und Praxis. ISR-Forschungsbericht Heft 49. Verlag der Österreichischen Akademie der Wissenschaften, Wien, pp. 109-129.
Year: 2019
Author(s): Kohlenberger, J, Buber-Ennser, I, Rengs, B, Leitner, S, and Landesmann, M.
Reference: Health Policy, Elsevier
Year: 2019
Author(s): Kohlenberger, J., Buber-Ennser, I., Rengs, B., Leitner, S., and Landesmann, M.
Reference: Gesundheitszugang von syrischen, irakischen und afghanischen Geflüchteten in Österreich: Ergebnisse aus dem Refugee Health and Integration Survey. In: M. Czaika, L. Rössl, F. Altenburg, A. Faustmann & T. Pfeffer (eds.), Migration und Integration 7: Dialog zwischen Politik, Wissenschaft und Praxis. Reihe Dialogforum Integration. Edition Donau-Universität Krems, Krems, pp. 239-259.
Year: 2019