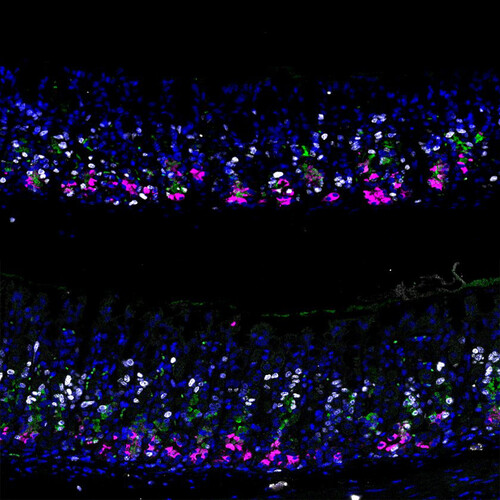
#ScienceChatIMBA: Double agents - How stomach stem cells change allegiance upon injury
Ji-Hyun Lee was interviewed by Daniel F. Azar (IMBA-GMI Communications & Partnerships).
Congratulations on this new publication, dear Ji-Hyun! What is special about the stem cell population you are studying?
(Ji-Hyun Lee, Postdoctoral Fellow in the Koo Lab): Thanks, Daniel. There is in fact an ongoing discussion among scientists regarding the roles and functions of adult stem cells. Many have believed that their only function is to proliferate and replenish the cells that make up an organ. However, increasing evidence demonstrates more complex functions of some of these stem cells. We are studying the stomach “chief cells”, a special adult stem cell population. These cells reside at the base of glandular structures that make up the tissue. We observed that these chief cells are reserve stem cells, meaning that their proliferation rate is very low under physiological conditions. Instead, they contribute to the stomach’s homeostasis, or normal physiological functioning, in that they have a secretory function and help with digestion.
Then what are the stem cell characteristics of these reserve stem cells?
Upon injury, these cells start rapidly proliferating and replenishing other cell types in the tissue. Hence, it appears that these cells get “activated” through injury. Therefore, we wanted to know why different adult stem cell populations have different characteristics, and why one of them can apparently change its allegiance from quiescent to active.
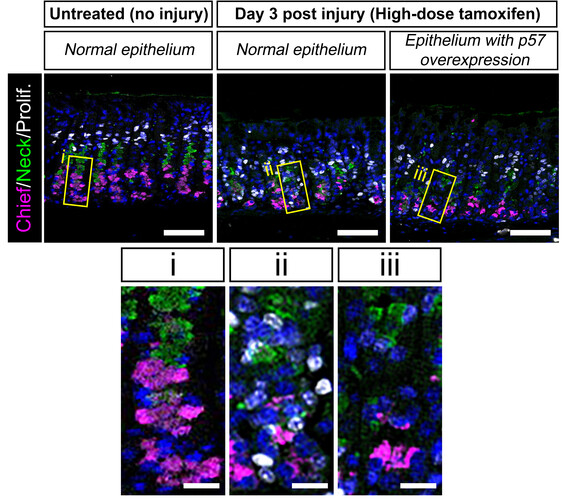
But is a change in the expression level of one molecule enough to speak of a “molecular switch”?
Of course not, as we needed to test that further and see if we could confirm these findings in other experimental setups. Indeed, we overexpressed p57 in stomach organoids. Organoids are usually highly proliferative because of the growth factor cocktail that they need in culture. However, once we introduced p57, the organoids suddenly stopped growing. We were thus able to induce a long-term reserve stem cell state in the organoids and an increased level of enzyme secretion. In a second step, we reduced the expression of p57, and to our delight, the organoids started proliferating again! This means that the cells did not lose their stemness due to p57. They merely went into a reserve state, exactly mimicking our in vivo observations.
This is great, but could you tell me more about p57? What does this molecule do, and does it belong to a broader family?
p57 belongs to the family of CDK inhibitors (cyclin-dependent kinase inhibitors). The members of this protein family inhibit the cell cycle and proliferation. Drugs with this function have been developed to treat cancer. Hence, we also tested the effect of other CDK inhibitors on stomach organoids. However, unlike p57, the other molecules did not induce a reversible reserve stem cell state in the organoids but simply caused them to die! With this, we were able to show that p57 is a gatekeeper and that it imposes the reserve stem cell state of the stomach chief cells during homeostasis.
Now that you have found the molecular switch, is there a way for you to use it?
Using the molecular switch in a clinical setting might be a little far-fetched, but it definitely teaches us a lot about existing gastric pathologies. One such known condition is called Spasmolytic Polypeptide-Expressing Metaplasia (SPEM), a chronic condition known to be pre-malignant. Also, there is evidence that SPEM originates from stomach chief cells. Although our experimental setup only allows us to test the effects of acute injury, we believe that a similar molecular mechanism is involved in this pathology. Hence, understanding the activation of chief cells ultimately helps us understand the underlying molecular mechanisms of SPEM.
Tell me about your general scientific interest. How did you come to work on the topic of quiescent stem cells and homeostasis?
I am interested in how the cells react in detrimental conditions, how they behave, and how they recover. Let me tell you something; what brought me to science was the idea of homeostasis itself. I felt like this phenomenon is very well coordinated and that the cells and tissues work as a computer system! I was indeed fascinated by this idea. I can say that I am quite driven by the natural characteristics of cells and the way they react to detrimental conditions. This interests me much more than cells that already have abnormal functioning. This probably explains why I research homeostasis rather than cancer!
Furthermore, let me finish by expressing my gratitude to our collaborators from Vanderbilt University Medical Center (Nashville, USA), and Pohang University of Science and Technology (POSTECH) (Republic of Korea). I would also like to acknowledge the two other co-first authors: Somi Kim, who handled the single-cell analysis, and Seungmin Han who initiated the project. I also thank my trainees who were as enthusiastic as myself with the project. I am very proud of having this huge collaborative effort on this paper and could not imagine leading such a project without their key contributions.